Key ways technology is transforming patient care in the NHS
Technology in UK healthcare is revolutionising patient care through the NHS digital transformation, leading to significant patient care improvements. The NHS has embraced multiple impactful technologies designed to enhance diagnosis, treatment, and overall patient experience.
One major advancement is the integration of electronic health records (EHRs), enabling clinicians to access unified patient data swiftly. This digital records approach ensures more accurate and coordinated care, reducing risks linked to incomplete information. Additionally, telemedicine UK services have expanded, allowing remote consultations that increase access and convenience, especially for those with mobility issues or during pandemics.
Also to see : How Can Innovations in Health Technology Improve Patient Engagement in the UK?
Artificial intelligence, a cornerstone of healthcare innovation UK, is another transformative force. NHS artificial intelligence programs support clinicians with AI diagnostics, improving the speed and precision of medical decisions. Pilot programs have demonstrated enhanced diagnostic accuracy and streamlined workflows.
Examples from leading NHS Trusts demonstrate how technology adoption improves healthcare outcomes UK. These include faster diagnosis, better resource allocation, and higher patient satisfaction. The NHS digital transformation is poised to continue evolving, with new tools advancing patient care improvements across the United Kingdom.
Have you seen this : What Are the Recent Innovations in UK Healthcare?
Electronic health records and data integration
Understanding electronic health records (EHRs) is central to grasping the NHS digital transformation. EHRs unify patient information, providing clinicians with rapid, comprehensive access to medical histories, test results, and treatment plans. This integration reduces errors from fragmented data and significantly enhances patient safety and care coordination.
In practice, NHS digital records systems facilitate seamless health information exchange between departments and Trusts, improving communication and continuity of care. For example, when patients move between specialists, their data travels with them in real-time, enabling informed decisions without repeated tests.
However, challenges remain. Interoperability issues arise due to varying software platforms across NHS facilities, complicating smooth data sharing. Data privacy and security are paramount, with the NHS investing in safeguarding patient information against breaches. Ensuring compliance with GDPR regulations maintains public trust while enabling data-driven improvements.
The combined benefits of EHRs have already demonstrated improvements in clinical workflows and patient outcomes. Through ongoing refinement of NHS digital records and robust health information exchange frameworks, the NHS is steadily advancing towards safer, more efficient, and patient-centred care delivery.
Telemedicine and remote care
Telemedicine UK has become a vital component of the NHS digital transformation, expanding access to healthcare through remote consultations. These NHS virtual care services enable patients to connect with clinicians from home, reducing travel time and wait periods significantly.
Remote consultations are now commonly used in both primary and specialist care, offering convenience without compromising quality. Patient feedback reflects high satisfaction levels, especially among those with mobility challenges or living far from medical centres. During the COVID-19 pandemic, the NHS rapidly scaled up telemedicine UK services, including remote monitoring for vulnerable patients. This approach provided timely care while minimising infection risks.
The broad adoption of telemedicine UK showcases real-world benefits like improved appointment attendance and faster clinical responses. However, it also highlights challenges such as ensuring reliable internet access and maintaining patient confidentiality during virtual visits. Overall, telemedicine UK is reshaping patient interactions within the NHS, driving forward more accessible, efficient healthcare delivery across the UK.
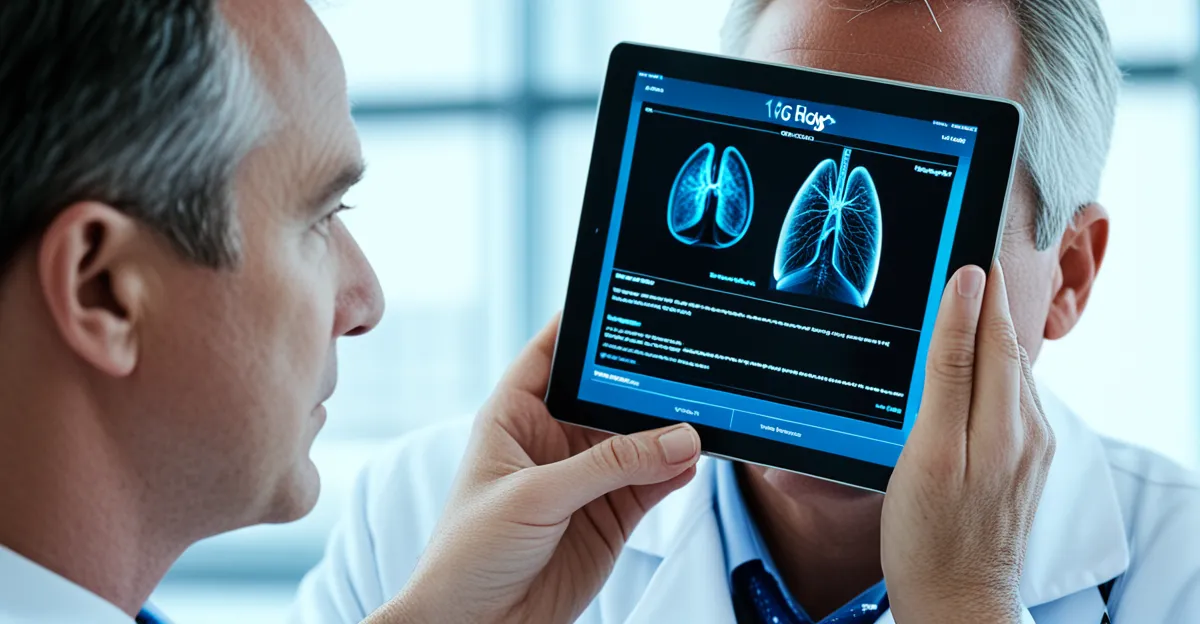
Artificial intelligence and advanced diagnostics
Artificial intelligence (AI diagnostics) is revolutionising patient care improvements within the NHS digital transformation. These NHS artificial intelligence tools provide clinicians with advanced diagnostic capabilities and real-time decision support, boosting both the speed and accuracy of medical assessments. By analysing vast data sets, AI diagnostics detect subtle patterns often missed by human eyes, leading to earlier disease identification and treatment.
NHS pilot programmes deploying AI diagnostics have shown promising outcomes, including improved detection rates for conditions like cancer and heart disease. For example, AI algorithms assist radiologists in interpreting imaging results more precisely, reducing diagnostic errors and unnecessary follow-up tests. These tools integrate seamlessly with existing NHS digital records, enhancing clinical workflows without disrupting patient care.
Beyond diagnostics, healthcare innovation UK through AI supports personalised treatment plans and optimises resource allocation. The NHS continues investing in AI development, focusing on safe, ethical deployment that complements clinicians rather than replaces them. While challenges such as data biases and model transparency exist, ongoing refinement aims to maximise benefits of AI diagnostics in improving healthcare efficiency and patient outcomes across the UK.
Efficiency, safety, and patient outcomes
The NHS digital transformation leverages technology in UK healthcare to markedly improve NHS efficiency, patient safety, and overall healthcare outcomes UK-wide. Automation has streamlined clinical workflows, with tools such as digital triage systems enhancing patient flow by prioritising cases based on symptom severity. This reduces waiting times and optimises resource allocation, ensuring timely care for critical patients.
Patient safety technology plays a pivotal role, integrating clinical alerts and error-reduction mechanisms within electronic health records and diagnostic platforms. These digital safeguards significantly lower incidences of medication errors and diagnostic oversights, directly benefitting patient outcomes. For example, alerts notify clinicians about harmful drug interactions or abnormal test results in real-time, preventing adverse events.
Documented improvements from NHS initiatives demonstrate the practical impact of these technologies. Many hospitals report reduced emergency department overcrowding and improved management of chronic conditions through continuous monitoring and rapid response systems.
Together, these advancements exemplify how embracing technology in UK healthcare supports safer, more efficient service delivery, ultimately driving enhanced patient care improvements across the NHS. Ongoing investment and refinement remain crucial to sustaining and expanding these benefits.